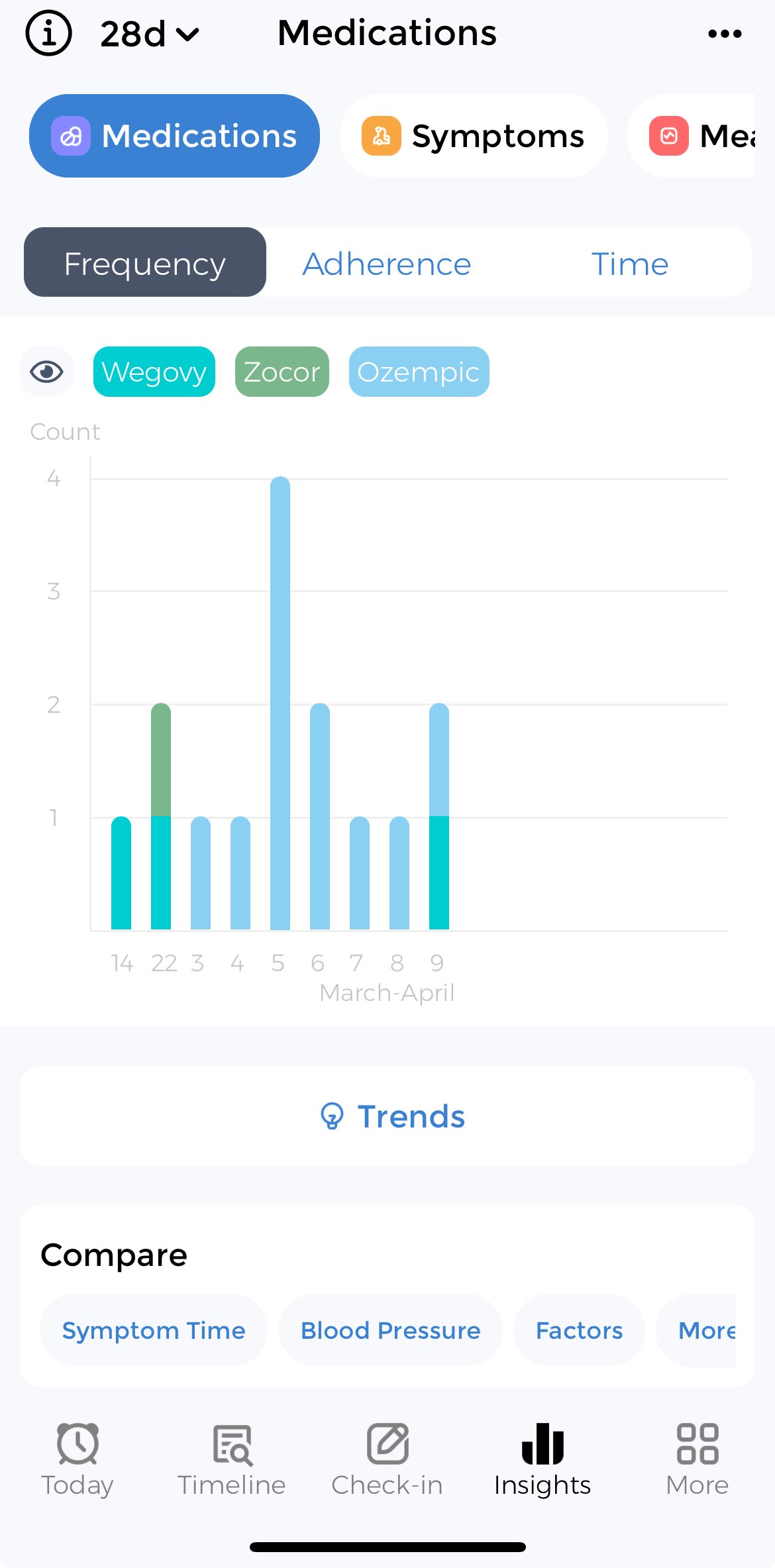
Medication Tracker
Get Reminders with Refill Alerts
Struggling to stay on top of your meds? CareClinic helps you track prescriptions, set reminders, and stay 100% consistent with your medication routine on iOS & Android.
Track All Medications
Medication Reminders
Pill Tracking Insights
Private and Secure
Why CareClinic Is the Best Medication Tracker App
Forgetting meds. Mixing up doses. Losing track of side effects. If you’ve felt this, you’re not alone. That’s why you need a real system, not sticky notes or guesswork.
Designed for Daily Use
- Track prescriptions, vitamins, supplements
- Log symptoms, side effects, reactions
- Set custom schedules for any medication type
Built-In Reminders and Refill Alerts
- Smart notifications that don’t let you forget
- Adjust times, repeat frequency, and snooze options
- Never run out with refill tracking

Who Should Use This Med Tracker?
Taking Multiple Medications?
CareClinic helps you organize all your meds, dosages, and schedules in one place. Ideal if you’re managing prescriptions for different conditions or doctors.
Caring for a Family Member?
Easily track medications for parents, children, or loved ones. Whether you’re a caregiver or a concerned family member, this app keeps you on top of everything.
Need a Simple Medication Log App?
Use CareClinic to log your pills, set refill reminders, and track any side effects. Perfect for anyone looking for a free, reliable way to stay consistent.
Want Better Control of Your Health?
Whether you’re starting a new treatment or just want peace of mind, CareClinic makes medication tracking stress-free and accessible from any device.
How to Track Medications Properly
Build Routines With Actionable Reminders
In CareClinic, reminders are linked to your care plan. You can connect doses with meals, sleep, or other habits to build stronger routines. Learn more about how to use a medication tracker here.
Track Side Effects With Context
CareClinic logs reactions alongside each medication entry. You can view patterns, add notes, and export everything for your doctor.
See What You Missed and Why
Beyond missed doses, CareClinic shows what else was going on that day. Stress, fatigue, travel, or pain are tracked to help you stay consistent.
Your Medication Journey with CareClinic
Start with a Care Plan
Create a personalized care plan that includes meds, therapies, and health goals.
Track Any Medication
Pills, injections, granules, OTC meds, supplements, vitamins – all covered.
Set Smart Reminders
Refill alerts, snoozing, custom time schedules, cycle tracking, and more.
Track Symptoms & Vitals
Monitor pain, mood, weight, BP, glucose and other metrics with context.
Manage Chronic Conditions
Stay on track with meds for mental health, heart, nausea, and other illnesses.
Prepare for Appointments
Bring reports for symptoms, meds, notes, immunizations, imaging, and labs.
CareClinic vs Other Pill Tracker Apps
Most health apps offer basic pill reminders. CareClinic combines medication tracking, condition management, wearable sync, and care coordination in one place. Compare features to see how we help reduce missed doses, simplify care routines, and increase long-term adherence.
Smart Reminders for Meds, Care Plans, and More
CareClinic makes it easy to manage your health routines across iOS, Android, iPad, tablets, and smartwatches. Get personalized alerts for meds, therapy, and lifestyle tasks from any device.
Medication-Based Reminders
Lifestyle & Care Plan Reminders
Track Your Medications by Condition with Full Control
Whether it’s ADHD meds, insulin injections, or hormone therapy, CareClinic gives you the tools to track, log, remind, and get medication notifications for everything you take—accurately and on time.
Track ADHD Medications & Improve Focus
Use CareClinic to log stimulant doses by time of day, track focus levels, and get silent reminders for morning and afternoon meds. Identify when your attention dips and adjust faster. Perfect ADHD tracker app for adults or teens.
Diabetes Medication Tracker with Glucose Logging
Log every injection, pill, and glucose reading in one place. CareClinic helps you correlate insulin timing with blood sugar levels before and after meals. Generate a diabetes medication log you can share with your endocrinologist.
Hormonal Birth Control Reminder App
Stay consistent with oral contraceptives or hormone replacement therapy. Set cycle-based reminders, track side effects like bloating or mood swings, and avoid missed pills. Includes IUD tracking and HRT dose history.
High Blood Pressure Medication Log
Pair BP readings with medication intake. Track when symptoms like dizziness or swelling appear after doses. Share your antihypertensive medication history with your cardiologist to avoid interactions and optimize timing.
Mental Health Medication & Mood Tracker
Record daily doses of SSRIs, antipsychotics, or mood stabilizers. Track mood, appetite, and sleep to identify patterns over weeks. CareClinic shows how your mental health meds correlate with lifestyle changes.
Post-Surgery Painkiller & Antibiotic Tracker
Log each pain med, anti-inflammatory, or antibiotic with time and dosage. Track nausea, pain scores, and tapering progress. Prevent missed doses and avoid overuse during recovery from surgery or injury.
Frequently Asked Questions About Our Medication Tracker
Wondering how a medication tracker app can help improve your routine, reduce missed doses, or manage care for a loved one? These are the most common questions patients and caregivers ask about staying consistent with treatment using CareClinic.