
Have Blood in Stool?
Hemorrhoids, also known as piles, are a cluster of pillow-like veins which lie under the mucous membranes that go around the lowest area of the rectum and the anus. Hemorrhoids are a condition that develops when those veins become swollen. This condition can result in symptoms such as pain when pooping and blood in stool (R)
You may be wondering, is pooping blood normal? Hemorrhoids are a common condition. In fact, almost three out of every four adults will have hemorrhoids from time to time. Fortunately, there are a number of effective treatment options for it. Furthermore, many people are able to find relief with home remedies and/or changes in their lifestyle.
Different types of hemorrhoids
There are 2 ways in which hemorrhoids can develop. Internal hemorrhoids occur in the lower rectum and develop inside the rectum. Usually, you cannot see nor feel them and they cause little discomfort. However, they may be irritated and in pain when pooping. The symptoms can be as follows:
- Noticing some bright red blood in stool
- Irritation and pain when pooping
What does pooping blood mean?
External hemorrhoids are painful because the skin over it can become irritated and eroded. You may feel sudden, sharp and acute pains if a blood clot forms inside of external hemorrhoid. You may notice external hemorrhoid when you see or feel a bump around or near the anus. The following symptoms may occur:
- Feeling itchy and/or irritation near the anal region
- Discomfort and/or pain when pooping
- Swelling around your anus
- Bleeding
In summary, hemorrhoids are bloated blood vessels that form either externally (around the anus) or internally (lower rectum).
Causes of hemorrhoids leading to blood in the stool
Generally, hemorrhoids are traditionally associated with constipation. Constipation is the straining during bowel movements, or prolonged time sitting on the toilet bowl. There is usually interference with blood flowing to and from the vessels in the anal canal. This blockage in blood flow can result in the vessels enlarging.
Recent studies have revealed that patients with hemorrhoids have a naturally tight anal canal. When compounded with constipation, this straining increases when there is a bowel movement.
The veins around your anus usually stretch out due to increased pressure which can lead to potential bulging or swelling. The following can lead to the development of hemorrhoids:
- Straining during bowel movement
- Spending lots of time on the toilet
- Having chronic diarrhea or chronic constipation problems
- Pregnancy
- Anal intercourse
- Low-fiber diet
- Regular heavy lifting
Risk factors
When you age, the risk of developing hemorrhoids increases because the tissues which support these veins in the rectum and anus regions may be weakened by stretching. This is something that can occur when you’re pregnant. The baby’s weight can add pressure and weight onto the anal region.
Health complications
Experiencing complications due to hemorrhoids is rare but can include the following:
- Anemia: Sometimes chronic blood loss from hemorrhoids can result in anemia. This is a condition in which there are not enough healthy red blood cells in the body.
- Strangulated Hemorrhoid: This occurs if the blood supply to an internal hemorrhoid is cut off, resulting in the hemorrhoid being “strangulated.” Such a complication can result in extreme pain.
- Blood Clot: Sometimes a blood clot can form in a hemorrhoid. Although it is not dangerous, it can be very painful and at times, may need to be treated and drained out.
Is there a connection between inflammatory bowel disease and hemorrhoids?
There is no known direct relationship between inflammatory bowel disease and hemorrhoids. However, both conditions can cause similar symptoms, such as rectal bleeding, anal pain, and itching. In some cases, people with inflammatory bowel disease may also develop anal fissures (small tears in the tissue around the anus), which can lead to hemorrhoids.
Can hemorrhoids block bowel movements?
Yes, hemorrhoids can block bowel movements. This is because when they swell, they can prolapse, or fall out of the rectum. This can cause a blockage that makes it difficult to have a bowel movement.
Diagnosing hemorrhoids
Usually, hemorrhoids can be easily diagnosed by checking the patient’s medical history and performing a physical exam. The external hemorrhoids are often very apparent, especially if there is a blood clot that has formed.
Digital examination
Your doctor may have to undergo a digital rectal exam in order to inspect blood in the stool. Your physician will administer this digital exam by inserting a gloved, lubricated finger inside of the rectum. This is done to check for unusual growth inside the rectum.
Visual inspection
As internal hemorrhoids are usually too soft to be felt in a rectal examination, your doctor may visually examine the lower portion of the colon and the rectum using a scope.
Your doctor may also request a colonoscopy if there are signs of other digestive diseases or risk factors for colorectal cancer. According to the Mayo Clinic, “colon cancer and hemorrhoids are both common conditions. However, the two are not related.” Colon cancer is a type of cancer that starts in the large intestine (colon). Hemorrhoids are swollen blood vessels in the rectum or anus. While hemorrhoids may cause bleeding, pain, and itching, they are not usually associated with colon cancer. However, both conditions can cause similar symptoms, so it is important to see a doctor for a proper diagnosis.
Colon cancer is the third leading cause of cancer death in the United States. If caught early, it is highly treatable, but it can be deadly if it spreads to other parts of the body. Hemorrhoids are very common, and they usually go away on their own. However, they can sometimes become painful and may require treatment. If you have any symptoms of either condition, it is important to see a doctor so that the cause can be properly diagnosed and treated.
Another thing to look into is colon polyps. A colon polyp is a small, benign growth that forms on the lining of the large intestine or rectum. Polyps are very common, with most people over the age of 50 having at least one. Although they are usually harmless, some types of colon polyps can develop into cancer over time. This is why it’s important to have any polyps that are found removed.
Prevention and home remedies for blood in stool
Some of the best ways to remedy as well as prevent hemorrhoid flare-ups can actually be found at home!
Following fiber-rich diet plans
By adding more fiber to your diet along with adequate amounts of fluids, your stool will soften and become easier to pass. This will thereby reduce pressure on hemorrhoids which will prevent flare-ups. Examples of high-fiber foods include:
- Broccoli
- Beans
- Wheat
- Oat Bran
- Whole-grain foods
- Fresh Fruit
High fiber food will also help reduce the irritation which can be invoked from smaller stools trapped around or near the blood vessels. Some people may find that as they increase their fiber intake, they may experience increased amounts of gas or bloating. It is best to take an incremental increase approach and to match the increase of fiber with increased fluid intake.
Increase fluid intake
Drinking six to eight glasses of water a day as well as other liquids help to keep stool soft.
Avoid long periods of sitting
Don’t stay seated for too long, especially on the toilet. This can increase the pressure on the veins in the anus.
Exercise
Moderate aerobic exercise, such as going for walks and or jogs (20~30 minutes per day), can increase the stimulation of bowel movement. This will lessen the strains on the vessels in the anus.
Go to the bathroom promptly
When there is the urge to pass stool, you should be heading to the bathroom immediately. This is because stool can pack up and result in increased pressure and straining. Establishing regular bowel habits are important. You may even choose to schedule a time of the day to go to the toilet for a few moments after meals.
Taking a sitz bath
The sitz bath refers to a warm water bath for the buttock region and hip area. The word ‘sitz’ comes from the German word “sitze” which means to sit. This warm bath can be utilized to relieve: itching, irritation and spasms of the sphincter muscle. The sphincter muscle hitch maintains natural constriction of the anal passage. Experts usually recommend taking a 20-minute sitz bath following bowel movement. It is also important to not rub and wipe hard following bowel movement after experiencing a hemorrhoid flare-up.
Pain Relievers
You can use certain medications such as acetaminophen (Tylenol and others), Aspirin or ibuprofen (Advil, Motrin IB) to relieve the occurrence of pain when pooping.
When to See a Doctor
If there is blood in stool or blood while wiping which do not improve after one week of home care, it may be time to visit your doctor.
Do not assume that the bleeding rectum is always due to hemorrhoids. This is especially something to be careful of if there has been a shift in stool coloration and consistency. Rectal bleeding has been attributed to other diseases like colorectal cancer and anal cancer.
Seek urgent medical care if there is a large amount of rectal bleeding or blood in stool, lightheadedness or dizziness.
Individuals with chronic constipation may strain too much during bowel movements and develop hemorrhoids. Hemorrhoids can cause small amounts of bright red blood clots in stool.
Little bleeding from hemorrhoids is not a major issue or a cause for concern, but a large amount of bright red blood in stool may indicate the need to contact your doctor. Large amounts of bright red blood in the stool can indicate the presence of damage in the intestinal tract. This requires immediate medical attention.
Bleeding in the stomach or intestines can cause darker poop. Therefore, dark blood in stool indicates bleeding in the upper digestive tract. This is because the blood has had enough time to travel through the digestive system, giving it a darker colour. Bright red blood may indicate bleeding lower in the digestive tract, which can be more serious. Consider tracking bowel movements in our app as well with photos to keep a log to be used later.
Medical procedures for hemorrhoid treatment
Sometimes there are cases in which home remedies cannot resolve hemorrhoids immediately. This can be due to various factors, including the persistence of symptoms or even the prolapse (the pushing out) of hemorrhoid itself.
There are a number of small treatment options which are less painful than a hemorrhoid removal (hemorrhoidectomy). These options also allow for faster recovery times. Such procedures are performed in a hospital by surgeons.
Non-Surgical Procedures
Rubber Band Ligation
This is a common hemorrhoid treatment method. It consists of using a small elastic band which is placed around the base of the hemorrhoid.
This band allows for the hemorrhoid to gradually sink as well as for the scar around the hemorrhoid to heal. It also holds the hemorrhoid in place. This usually takes between four and six procedures which are done between six to eight weeks apart in order to eliminate the hemorrhoid.
There can be complications that arise including some mild pain, tightness and bleeding. A sitz bath can be done to resolve most of these complications. The rubber band ligation is useful, but there are potential side effects and the possibility of recurrence. However, each situation is different.
It is recommended that you discuss with your doctor regarding the best course of action for you.
Injection (sclerotehrapy)
Your doctor in this case will inject a chemical solution into the hemorrhoid’s tissue to shrink it.
The injection itself will result in little or no pain but it may be less effective than rubber band ligation.
Coagulation (Infrared, Laser, Bipolar)
Coagulation techniques usually rely upon laser, infrared light and/or heat. They cause internal hemorrhoids to harden and shrivel. Coagulation has relatively fewer side effects and rarely causes any discomfort.
Abdominal pain from hemorrhoids, is it possible? and what to do?
Yes, it is possible to experience abdominal pain from hemorrhoids. Several things can cause this pain, such as inflammation, straining during bowel movements, or sitting for long periods. If you are experiencing abdominal pain from hemorrhoids, there are a few things you can do to ease the pain. Taking over-the-counter pain medication, applying a hemorrhoid cream or ointment to the affected area, and drinking plenty of fluids can help. If the pain is severe, you may need to see a doctor for treatment.
Surgical Procedures
Hemorrhoidectomy
Surgery is usually reserved for larger hemorrhoids that have not responded to other forms of treatment. Usually, only a small number of patients referred to coloproctologist for hemorrhoid treatment ever receive surgery.
Surgical hemorrhoidectomy is usually quite painful and it is generally performed in a day care basis. It’s important to have a pain relief package in order to reduce pain, this concludes anesthetics, analgesics and laxatives to reduce pain post-operation. It’s important to take note of potential complications as a result of surgery.
Stapling
The stapling procedure is a method that blocks the flow of blood to the enlarged and swollen hemorrhoidal tissue. It is typically used for internal hemorrhoids.
The stapling method is usually less painful than the hemorrhoidectomy and it allows for an earlier return to regular activity. However, in comparison to surgical hemorrhoidectomy, it actually has a greater chance of recurrence and even rectal prolapse (the protrusion of the rectum from the anus).
There are also other complications that may arise. These include rectal bleeding, urinary retention and pain at times. Very rarely, there could also be a blood infection (sepsis).
CareClinic always recommends you consult your doctor in order to find the best option for your situation.
Keeping Track with CareClinic
The best way to prevent blood in stool and a potential trip to the doctor is by preventing the development of your hemorrhoids. There are a variety of ways to prevent blood in stool.
Tracking a healthy and following fiber rich diet plans
Ensure the prevention of future flare-ups by simply maintaining a fiber-rich diet plan. CareClinic’s all-in-one health management platform is an effective way to ensure you are adhering to your fiber intake goals. Nutrition can be tracked daily and you can see if you are meeting your unique health goals at any time.
Track blood in stool and other symptoms
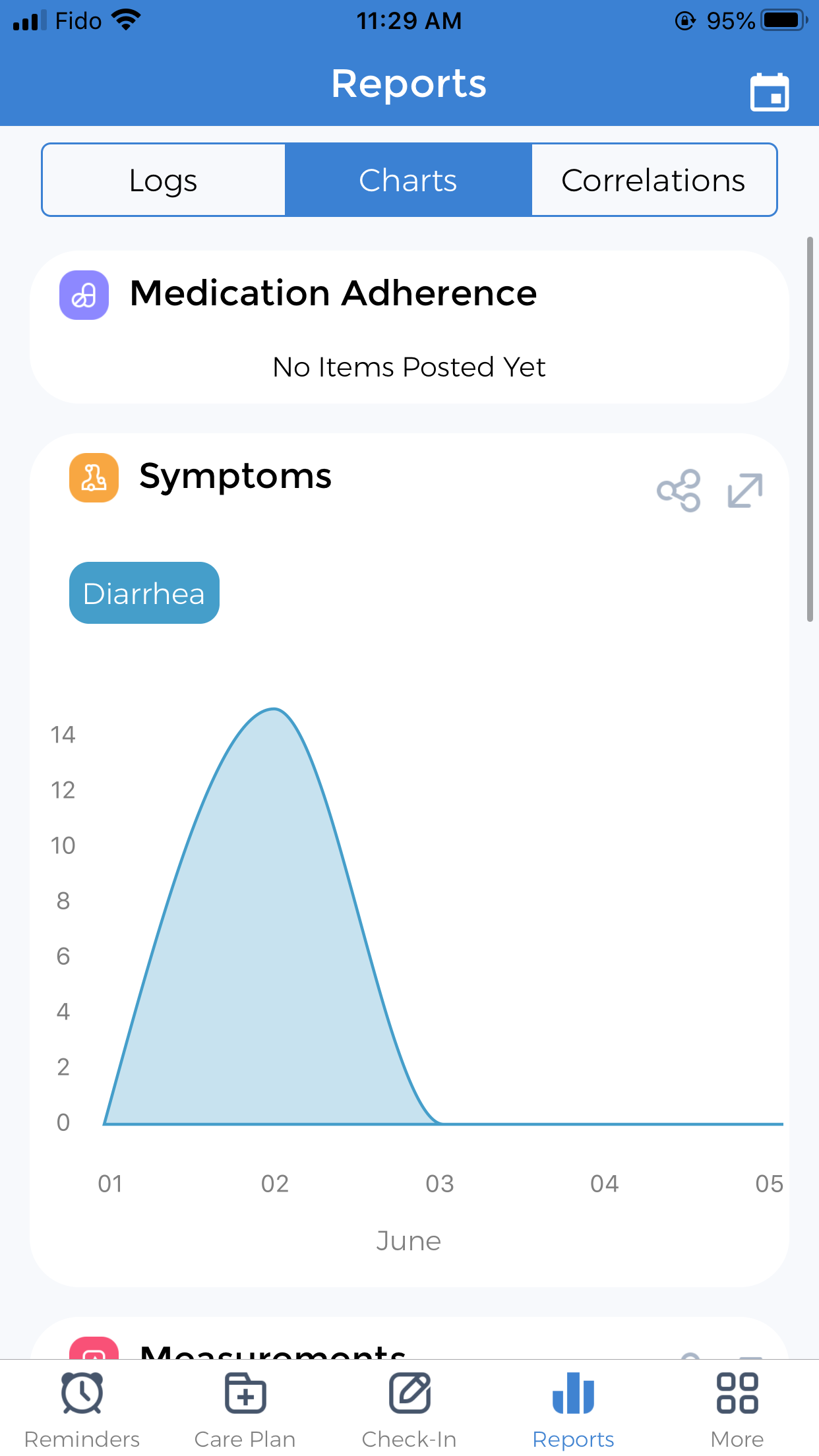
CareClinic’s care plan is an all-inclusive way for you to track your symptoms and other aspects of your wellness. You can keep track of the medicine that you are taking for your hemorrhoids, your physical activity plan and your nutritional plan. Additionally, use the app to track your symptoms such as the occurrence of blood in stool, rectal bleeding and pain when pooping.
You can also jot down any ideas or recommendations you have received for foods to help with constipation. Use the app to easily take note of any home remedies blood in stool. If you experience constipation and/or chronic diarrhea, this can be tracked with the Symptom Tracker. This way, a visit to the doctor can be fruitful as you now have an accurate recount of all your symptoms and issues on a daily basis!
Continue to stay active
One of the main causes of hemorrhoids is closely related to staying seated for long periods of time. It is crucial to stay active. This can relieve the stress and pressure on the anus. You can use the CareClinic app to add and track your daily activity. You can create an activity plan and ensure that you stick to it. Daily check-ins with the Care Plan is a great way to do so!
Stay in contact with your care team
If you frequent a family doctor, local clinician or caregiver, it is important that they are kept updated on your situation. Through the intuitive and easy-to-use CareClinic app, you can add your caregivers to your Care Team on the app. During the recovery process, it’s extremely important to keep your doctor updated on side effects, feelings of pain when pooping, recurrences down the line and general discomfort. You can share all of this information easily through the CareClinic app. Communication with your doctor and family is made easy and consistent with CareClinic.
Maintain a healthy fluid intake
It sounds simple enough, but the importance of fluid intake (six to eight glasses daily) cannot be overstated. This, combined with a healthy, fiber-rich diet plan, means that it will be a lot easier to pass stool when needed. These lifestyle changes will effectively lower the occurrences of constipation, pain when pooping and strain on the rectum area during trips to the bathroom.
The CareClinic app can assist with tracking your fluid intake and occurrences of constipation or blood in stool. This information can easily be shared with healthcare practitioners at any time and place. Individuals can also use this information to make the necessary changes to their lifestyle.
CareClinic, a free health app to help manage blood in stool
Hemorrhoids do not develop over one or two days. Build up in straining, pressure and added weight on the anal region cause the flareup of hemorrhoids. This is also why sometimes it is more common for older adults to experience hemorrhoids as they spend a longer amount of time sitting.
CareClinic’s user-friendly platform is a great way to keep track and manage your health with regard to hemorrhoids. In the unfortunate case that your hemorrhoid does flare up, the CareClinic app is always here to suit your every need with end-to-end support from designing a custom care plan to connecting you directly with your doctor! It is free to download on iOS and Android. The app can help with effectively reducing the occurrences of blood in stool and pain when pooping.
Here is a quick video about the causes of blood in stool and how to deal with it:


